COVID-19: A Bad Scar on Surgical Activity
Armel Ngami, PhD; Pierre Net, PharmD; Florent Guelfucci, PhD; Florence Bianic, MSc, Syneos Health, Value Access & HEOR, Montrouge, France; Louise Parrenne, PharmD; Franck Le Mercier, PharmD; Anne Lecoeur, PharmD, Hôpital Ambroise Paré AP-HP, Service Pharmacie, Boulogne, France; Léo Cazin, MSc, Hôpital Ambroise Paré AP-HP, Direction des Opérations et de la Performance, Boulogne, France
Introduction
The COVID-19 outbreak in early 2020 overwhelmed healthcare systems worldwide. Following the first cases detected in Wuhan, China, the Sars-CoV-2 spread swiftly across the globe, infecting millions of individuals in record time. Hospitals were quickly overloaded due to the resulting surge in activity, and healthcare professionals had to adapt their practices to face the crisis.
When facing a sudden increase in patient influx, one common response for hospitals is to postpone or cancel surgeries so that staff and equipment can be reallocated to intensive care units. However, when used over long periods of time, this strategy can lead to delays in diagnosis and treatment, resulting in significant losses of chance for patients. Considering the pandemic is still ongoing, it can be expected that COVID-19 is responsible for a substantial indirect health burden represented by postponement or absence of appropriate care in time.
A national lockdown was declared in France on March 16, 2020, and soon after, the Ministry of Health and regional health agencies issued a list of interventions that were considered urgent and interventions that could be delayed.1,2 We conducted a study to assess the impact of COVID-19 on surgical activity, leveraging data from a university teaching hospital located in Paris, France. Following the recommendations from the Ministry of Health, we assumed urgent surgeries would not be impacted by the pandemic while nonurgent surgeries would either be delayed or canceled."The study focused on 3 time periods corresponding to the lockdowns that were implemented in France in March 2020, October 2020, and April 2021."
Assessing the impact of COVID-19 on surgical activity
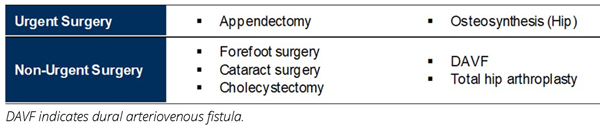
The study was conducted in a French university teaching hospital of 400 beds equipped with 10 operating theaters and performing more than 17,000 surgeries per year. All surgeries for the period between January 2017 and April 2021 were extracted, and 7 surgeries of interest were considered and labeled as urgent and nonurgent by the authors (AL, LP, and PN) (Table 1). The study particularly focused on 3 time periods corresponding to the 3 lockdowns that were implemented in France in March 2020, October 2020, and April 2021. We assumed those periods would be associated with high COVID-19 activity levels, translating into a decrease in activity for nonurgent surgeries and a steady activity regarding urgent surgeries. The weekly count of surgeries was analyzed using statistical models that account for the time dimension within the data in order to measure the effect of COVID-19–related lockdowns on surgical activity.
Table 1: COVID-19–related lockdowns were associated with a decrease in surgical activity and especially nonurgent surgeries.
Our results indicate that lockdown periods were associated with a significant decrease (-24%) in overall surgical activity (Figure 1, Table 2). This decline was mainly represented by nonurgent surgeries (consistent with the recommendations), and the weekly number of hip arthroplasty, forefoot, and cataract surgeries dropped by 38%, 48% and 64%, respectively. These results were in line with our initial hypothesis and show that COVID-19–related lockdowns were associated with a decrease in surgical activity and especially nonurgent surgeries. The decrease in activity can be explained by the fact that equipment and staff were re-allocated to treat COVID-19 patients. Particularly, ventilators were on high demand to treat severe COVID-19 patients while additional skilled personnel were required to perform and monitor intubations.
Figure 1: Evolution of surgical activity from 01/2017 to 07/2021 (all surgeries).
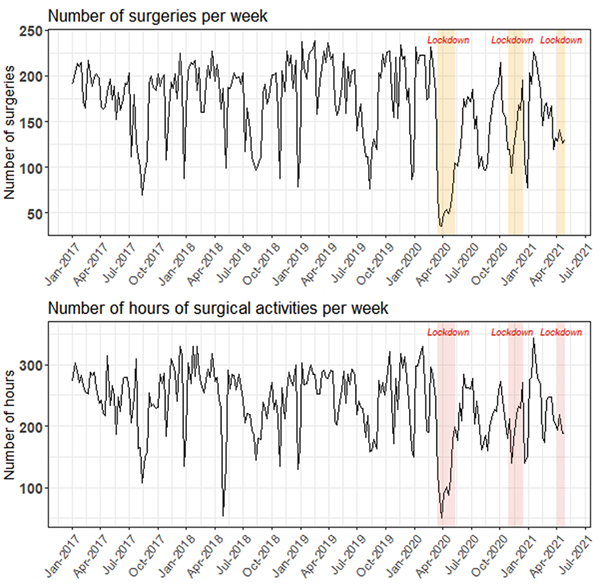
Table 2: Impact of lockdowns on surgical activity.
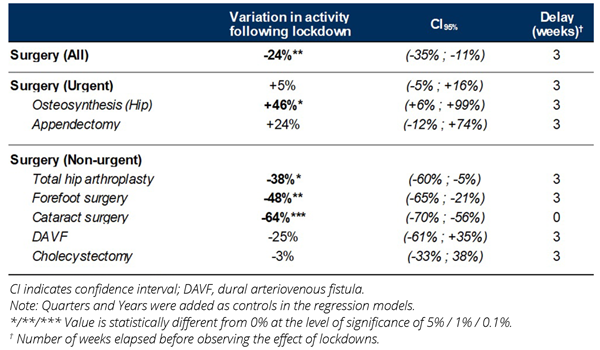
Inversely, increases in urgent osteosynthesis (hip) activity (+46%) and appendectomy (+24%) were observed, although results for the latter were not significant (Table 2). Results for urgent osteosynthesis (hip) can partially be explained as the hospital where the study was conducted specialized in orthopedic surgery, and it is possible that patients from nearby structures were transferred there to be treated. Another element to consider is that lockdowns may have been associated with increased risk of hip fractures, especially in elderly populations. As movements and services were limited during lockdown periods, it is possible that elderly had to take on more tasks than usual, translating into higher risks of falls and fractures. Additionally, it is likely that lockdowns were also responsible for physical inactivity, which is a risk factor associated with falls.3 However, opposite results were reported in the literature and particularly in Paccou et al who concluded to a reduction in hospitalizations for hip fractures of 11% during the first lockdown compared to a similar time period in 2019.4 The study was also conducted in France and leveraged the French national hospital database, gathering a total cohort of 91,160 patients. Although the results from Paccou et al should be kept in mind, they cannot be directly compared to ours because the authors focused on the first lockdown while we considered all 3 lockdowns. As such, further research is needed to confirm our hypothesis. Finally, we noted the effects of lockdowns on surgical activity were not observed immediately, but on average, with a 3-week delay (all lockdowns considered). Although our study considered a monocentric setting, the selection of a large time horizon and control period (4 years and 3 years respectively) brings a sound robustness to our results.
"Results indicate that lockdown periods were associated with a significant decrease (-24%) in overall surgical activity, especially nonurgent surgeries."
One limitation of our work is that patient transfers across hospital were not taken into account. Indeed, patient transfers were common during the pandemic to reduce the strain of the pandemic on highly affected geographical areas like the Paris region. A second limitation lies in the choice of surgery types selected for this study. The study center being highly specialized in orthopedic surgery, most of the included surgeries were related to this specialty, and hospitals specialized in different areas might not show similar results.
This work represents a first step in assessing the indirect burden caused by the pandemic and one immediate step would be to translate the decrease in surgical activity into monetary value by linking hospitalization costs to our results. More challenging research would involve assessing the impact of delays on quality of life and involve clinicians in extrapolating what could have been the consequences in terms of disease progression and/or loss of chance for patients. Ultimately, our insights advocate for broadening the scope of indirect burden and not limit it to wage loss as is commonly seen in economic evaluations. Expanding the scope of indirect burden could be considered in future health economic evaluations related to infectious diseases susceptible to overload healthcare systems such as COVID-19, influenza or, respiratory syncytial virus and would allow for further reinforcing the value of vaccination.
Looking ahead
To this date, the COVID-19 pandemic is estimated to be responsible for more than 22 million cases and 100,000 deaths in France.5 Although this direct burden is important, it can be assumed that the virus is linked to an equally significant indirect burden, delays in surgery being one aspect of it. Delays will probably have a substantial impact in the near future as patients who required intervention would see their conditions progress and/or deteriorate. In our study, it is likely that delays in forefoot surgery or total hip arthroplasty translated into reduced mobility and additional pain for patients, ultimately leading to a degraded quality of life for an extended period of time.
A similar observation can be made regarding delays in diagnosis as the CDC has already observed a drop in cancer screenings of 87% for breast cancer and 84% for cervical cancer in April 2020 compared to the previous 5-year averages.6 The health and economic consequences of delays were modeled in a UK study that estimated delays in diagnosis for 4 different cancer sites (breast, colorectal, esophageal, and lung cancer) following the first COVID-19 wave would result in 32,700 QALY and £103.8 million lost in the next 5 years.7
"This work represents a first step in assessing the indirect burden caused by the pandemic. One immediate step would be to translate the decrease in surgical activity into monetary value by linking hospitalization costs to our results."
Delays will also take time to resorb, translating into longer waiting lists for patients and additional and continued efforts required from healthcare professionals. Furthermore, many individuals have developed a fear of the virus over the pandemic and have avoided contacts with healthcare professionals and would then need to be encouraged to swiftly seek care again.8
Although literature on this topic is continuously being added, delays in surgery and diagnosis only represent a proportion of the indirect health burden of COVID-19 and future research should also focus on other areas such as the impact of COVID-19–related lockdowns on physical/mental health/education and consequences on healthcare providers.
References
1. ARS. Recommandations régionales COVID-19 - Période de déconfinement. 2020.
2. ARS. Recommandations régionales COVID-19 - Prise en charge chirurgicale. 2020.
3. De La Cámara MÁ, Jiménez-Fuente A, Pardos AI. Falls in older adults: the new pandemic in the post COVID-19 era? Medical Hypotheses. 2020;145:110321.
4. Paccou J, Lenne X, Ficheur G, Theis D, Cortet B, Bruandet A. Analysis of hip fractures in France during the first COVID-19 lockdown in spring 2020. JAMA Netw Open. 2021; 17;4(11):e2134972.
5. Santé Publique France. InfoCovidFrance. Chiffres clés et évolution de la COVID-19 en France et dans le Monde [Internet]. https://www.santepubliquefrance.fr/dossiers/coronavirus-covid-19/coronavirus-chiffres-cles-et-evolution-de-la-covid-19-en-france-et-dans-le-monde. Accessed April 1, 2021.
6. Sharp Declines in Breast and Cervical Cancer Screening. Centers for Disease Control and Prevention. https://www.cdc.gov/media/releases/2021/p0630-cancer-screenings.html. Accessed April 27, 2022.
7. Gheorghe A, Maringe C, Spice J, et al. Economic impact of avoidable cancer deaths caused by diagnostic delay during the COVID-19 pandemic: a national population-based modelling study in England, UK. Eur J Cancer. 2021;152:233–242.
8. Taylor S, Landry CA, Rachor GS, Paluszek MM, Asmundson GJG. Fear and avoidance of healthcare workers: an important, under-recognized form of stigmatization during the COVID-19 pandemic. J Anxiety Disord. 2020;75:102289.

