Increased Access at Lower Cost: Multilevel Insurance Plans in China
Martin Vu, MPH, BSc; Koen Degeling, PhD, MSc, BSc, Cancer Health Services Research, The University of Melbourne, Melbourne, Australia
Recent and ongoing healthcare reforms in China have increased policy coverage and drug reimbursement, while decreasing the budget surplus from 24.6% in 2010 to 4.5% in 2019. Despite these achievements, out of pocket costs to patients and access to innovative therapies remain important challenges. This session discussed how public and private insurers and manufacturers can work together through so-called multilevel insurance plans to address these challenges.
Rising to the Challenge
China has made significant strides to expand access to medical care and drugs through centralizing the drug negotiations setting, leveraging existing purchasing power, annual revisions to the National Reimbursement Drug List and unifying basic healthcare insurance coverage between urban and rural residents. [Figure 1] According to Mingqiang Li, PhD, Taikang Insurance Group, Beijing, China, these policies have reduced drug costs and increased consistent policy coverage for patients across China. However, increased growth in healthcare expenditure and sustainability of the healthcare system in China remain a significant policy concern. Furthermore, substantial out-of-pocket costs to patients and access to effective innovative therapies with high costs are continuing challenges.
Figure 1. Impact of multilevel insurance plan on healthcare coverage.
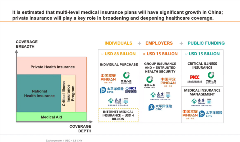
To overcome challenges, the government is encouraging private insurers and alternative funding sources (such as charity foundations and manufacturers) to play a pivotal role in the long-term sustainability of the healthcare system through multilevel insurance plans.
From Need Comes Opportunity
Discussion leader Monica Martin De Bustamante, AB, BE, CBPartners, New York, NY, USA asked the audience what they considered to be the greatest opportunity and challenge associated with multilevel insurance plans in China. The large size of the market and potential patient pool was considered the biggest opportunity (43%), followed by government policy support (29%), and addressing unmet clinical and financial needs (21%). The audience considered a lack of in-depth and systematic collaborations to be the biggest challenge (67%), followed by limited and high risk in coverage for rare diseases (20%), as well as a limited data tracking infrastructure (13%). [Figure 2]
Figure 2. Opportunities and challenges for multinational manufacturers in establishing China’s multilevel insurance plan.

According to Wahseng Lim, PhD, MBA, Takeda China in Beijing, private health insurance in China has evolved from a diagnosis-driven lump-sum payment to a high-deductible health plan in which insurance plans cover general disease and critical illnesses. To further increase access to healthcare technologies and reduce out-of-pocket costs, specialty drug insurance has been introduced to cover common cancer and non-National Reimbursement Drug List targeted therapies. This program goes beyond care reimbursement, aiming to serve as a one-stop solution for cancer diagnosis and management, for example, by providing patients with recommendations regarding suitable clinical experts and direct payments to pharmacies and guaranteed medicine supplies. Ultimately, private insurers will work together with public payers to design health plans and take on administrative tasks, such as the management of chronic illnesses and performance-based contracts with healthcare providers.
"Private health insurance in China has evolved from a diagnosis-driven lump-sum payment to a high-deductible health plan in which insurance plans cover general disease and critical illnesses."
—Wahseng Lim, PhD, MBA
Reducing Economic Burdens
From a manufacturer point of view, Dr Lim discussed 4 promising programs that are being piloted to further reduce the economic burden to patients:
- Local public payers channeled funding for which municipal funds, charity foundations, and manufacturers work together
- Public payers provided policy guidance and collaboration with private insurers to design supplementary insurance coverage
- Insurance schemes co-designed by manufacturers and private insurers, leveraging the knowledge and experience of both parties
- Collaborations between local charity foundations and manufacturers on patient assistance programs to improve patient access
All these developments show promising outcomes and demonstrate the continuing efforts to reduce out-of-pocket costs for patients and improve access to new and expensive healthcare technologies in China.
What Lies Ahead
As observed by Gordon G. Liu, PhD, National School of Development, Peking University, Beijing, China, reshaping the future healthcare system landscape in China will require increased utilization of big data to better inform decision makers on changes to market demands and funding capacity. This is in addition to other observed trends associated with government policy guidance, such as building on a strong healthcare service provider network to more effectively integrate and coordinate healthcare services.
Leveraging additional funding sources and continued expansion of healthcare insurance coverage policies—from traditional payment models to multilevel insurance plans—will become critical in ensuring that patients in China gain affordable early access to new and emerging healthcare technologies, while maintaining a healthcare system that can appropriately respond to the medical needs of patients across the country.

