Health Technology Assessment: Challenges and Lessons Learned in Asia
Cate Bailey, PhD, MApSci, BA; Monash University, Melbourne, Australia; Ingrid Cox, MD, MSc, Dip, University of Tasmania, Hobart, Australia
Health technology assessment (HTA) from a single payer or decision-maker perspective has historically made the process easier and more impactful. However, many countries have complex health systems that incorporate both public and private partners, run parallel health systems, or systems that run at a regional and national level. Today’s panelists discussed some of the challenges of conducting and using HTA in healthcare systems with multiple payers with perspectives from 3 Asia Pacific countries: China, India, and Thailand.
HTA in the Region
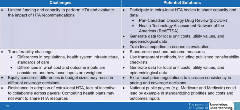
To set the stage, Naoko Ronquest, PhD, RTI Health Solutions, Durham, NC, USA, provided some results from a recently completed systematic literature review conducted by the ISPOR HTA Council Working Group. [Figure 1] Although the review took a global perspective, Dr Ronquest focused on some of her results applicable to the Asia Pacific region. Most of the challenges identified from a global perspective were also applicable to Asia. These included limited capacity and funding to conduct and implement HTA; issues of transferability across populations, health systems and standards of care; equity concerns; and resistance to the adoption of HTA when it was extra-local. Potential solutions were participation in extra-local bodies to share capacity and data, alongside generating local data and building local exercise in economic evaluation. The key to streamlining HTA in Asia was methodological standardization, local data and HTA talent generation, and cross-regional market collaboration and sharing,” Dr Ronquest concluded.
Figure 1. Proposed challenges and solutions highlighted from the ISPOR Working Group on HTA Literature review

In India, HTA is recognized as an important tool for improving resource allocation efficiency. Although India has a universal health coverage agenda, Devarshi Bhattachanryya, BDS, MSc, MPH, Eli Lilly and Company, Bengaluru, India, stated that the Indian health system is a microcosm of all the world’s healthcare systems. The health system includes multiple government payers from central and state governments, multiple stakeholders, a dominant private healthcare system, as well as high rates of out-of-pocket expenditure of around 60%. An outline of the Indian healthcare system is shown in Figure 2.
Figure 2. Outline of the Indian Healthcare System
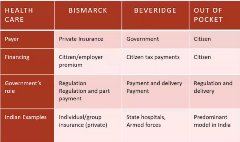
Government expenditure on the health system in India is low, and currently around 1% of the GDP (gross domestic product). Prices of innovative drugs are set by pharmaceutical companies without the requirement of an HTA assessment, leading to low access of these medications in India. There is a recent focus on moving from provider to payer decision making, with a focus on uniform HTAs that would be applicable throughout the country. When asked about how best to harmonize across private and public settings, Mr Bhattachanryya said:
“I think this is something we are learning currently. You need to stick to a national plan so that at least you have something as a framework. Willingness-to-pay thresholds in a country like India is also an issue because some of the states have higher willingness to pay than some of the other states but initially it makes sense to have a national plan and then try to tailor to different states.”
—Devarshi Bhattachanryya, BDS, MSc, MPH
Yingyao Chen, PhD, Fudan University, Shanghai, China provided an overview of the complexities of the Chinese Health System and the resultant increasing expenditure. The main challenge was that HTA was a developing discipline, with a lack of clear national guidance on appraisal processes or guidelines. In addition, there is limited capacity to conduct HTA among the varying stakeholders. He concluded that the key to HTA in China was to embrace “pluralistic systems that encompasses central and local payers and public and private payers” and encourage private insurance as a supplement to government insurance. Given the varying contexts of Asian countries, he emphasized that a standard can be established for all countries in the region and then establish a China-specific HTA mechanism and system to inform national level reimbursement decision making.
Thailand has 3 main health insurance schemes, with universal coverage for 75% of the population, and employer and civic service schemes for 15% and 10%, respectively Nathorn Chaiyakunapruk, PharmD, PhD, Department of Pharmacotherapy, University of Utah, Salt Lake City, UT, USA, discussed some of the issues with delivering HTA in the Thai context, echoing the results from the previously mentioned ISPOR HTA Council Working Group systematic review. These issues included limited HTA capacity in terms of human resources, limited budget, and transferability. Collaboration across systems and good governance were some of the lessons learned in Thailand. Dr Chaiyakunapruk emphasized methodological standardization as an important factor.
In conclusion, there was a general consensus from the panelists that leadership, good governance, and working together would be helpful in building HTA capacity across the Asia Pacific region. [Figure 3]