A Look at Added Therapeutic Benefit Assessments
Section Editors: Soraya Azmi, MBBS, MPH, Beigene, USA; Agnes Benedict, MSc, MA, Evidera, Budapest, Hungary
Assessing the Added Therapeutic Benefit of Ultra-Expensive Drugs
DiStefano MJ, Kang S-Y, Yehia F, Morales C, Anderson GF
Value Health Regional Issues. 2021;24(3):397-403.
Added therapeutic benefit (ATB) assessment relies on gauging the value of a drug or technology through improvement in patient-relevant endpoints. Valuation of medical technologies and drugs guided by assessment is often a first step in the reimbursement process. It could present an alternative to cost-effectiveness analysis for jurisdictions where it is not acceptable, as it is less tied to income and willingness-to-pay levels.
Adoption of the ATB assessment to inform the reimbursement and pricing process becomes relevant especially in the case of extremely expensive drugs, which can lead to a significant cost burden for the payers. This paper examined the added therapeutic benefit of the most expensive drugs prescribed to Medicare Part D beneficiaries in the United States by utilizing publicly available ATB ratings from the health technology assessment agencies in France, Germany, and Canada. These countries have similar gross domestic product to the United States, and ATB ratings are assigned independent of the drug price and the therapeutic benefit compared to the current standard of care. The factors considered in ATB assessments across the 3 countries were (1) quality of research evidence; (2) improvement in efficacy; (3) clinical relevance; (4) assessment of innovation; (5) patient and caregiver convenience; and (6) reduction in incidence and side effects, among others.
Drugs were considered “ultra-expensive” when the average annual per beneficiary spending by Medicare Part D program in the United States was greater than the per capita gross domestic product of the United States in 2018 ($62,794). This threshold is somewhat arbitrary but is only used by authors to select the therapies that they later analyze from the perspective of ATB.
As a result of the varying rating mechanisms across France (5 levels of ATB: major, important, moderate, minor, and none), Canada (4 levels of ATB: breakthrough, substantial, moderate, and slight/none), and Germany (6 levels of ATB: major, considerable, minor, nonquantifiable benefit, none, and less) a binary variable was created that collectively classified the top 2 levels in each of the countries as ‘‘high ATB” and the rest of the levels were defined as “low ATB.”
A modification to this variable was made for Canadian assessments conducted prior to 2010 as they had defined only 3 levels of ATB (breakthrough or substantial, moderate/little/none, and a line extension). Drugs classified as breakthrough or substantial were termed by the authors as ‘‘high ATB” whereas the remaining were categorized as “low ATB.”
A total of 122 drugs were defined as ultra-expensive, 79% of which were approved as orphan drugs in the United States with an average amount of $174,669 annual spent per Medicare beneficiary. Not all of these were assessed internationally: 60% were assessed in France, 45% in Canada, and 35% in Germany (Figure).More than 70% of the drugs assessed in France (85%), Canada (73%), and Germany (74%) received a low ATB rating. Around 93% of drugs analyzed within 1 country and 61% of drugs assessed in either 2 or all 3 countries were classified as contributing low ATB in comparison to the existing standard of care.
None of the drugs evaluated in all the countries were rated as high ATB. There was a high agreement in scoring between France and Canada (85%), followed by Canada and Germany (69%), and France and Germany (67%). Around 67% of the assessed drugs in France and Canada, 62% in Canada and Germany, and 67% in France and Germany were always rated as low ATB (ie, there was relatively consistent assessment across countries. None of the drugs were always rated as high ATB in France and Germany). Despite the low ratings of many drugs, the per capita Medicare spending for each is high, indicating that a substantial proportion of the spending covers for drugs with low ATB. The authors were especially concerned that over 70% of the drugs assessed in the study were categorized as orphan and were priced at a much higher rate but offered a lower ATB in comparison to the likely much less expensive standard of care.
This paper highlights a potential first step towards value-based pricing in the United States: ATB assessment does not depend on the quality-adjusted life-year or the use of a value threshold, it may be more politically acceptable than cost-effectiveness analysis. Although the implementation of ATB and its position along the reimbursement pathway is different across the 3 countries (eg, pre- or postmarket entry), the authors suggest that the ATB assessment of either Germany, France or Canada could serve as a proxy until there are US-specific ATB criteria.
With the number of ultra-expensive therapies growing and the proportion of public health expenditure spent on these increasing, there is a greater need for resource allocation decisions that may be potentially more equitable and could provide care for more patients in the United States. The authors present some convincing arguments as to why it may be time to consider examples, even when cost-effectiveness analysis is not politically desirable. •
Figure 1. Percentage of ultra-expensive drugs per added therapeutic benefit score by country. The “low ATB” category includes ratings of “no ATB,” but we distinguish them here for purposes of interpretation. The Canadian rating system does not provide assessments at this level of granularity.
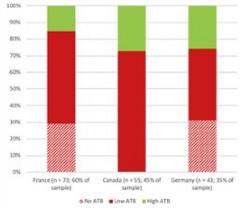
ATB indicates added therapeutic benefit.

