HEOR Studies in Medication Management
Jacinda N. Tran, PharmD, MBA, The Comparative Health Outcomes, Policy, and Economics (CHOICE) Institute, Seattle, WA, USA
Health economics and outcomes research (HEOR) leverages a wide range of methods to describe, understand, and optimize effectiveness and cost-effectiveness of medication management. In this podium presentation session, HEOR is used to evaluate a medication synchronization intervention, characterize pharmacist-administered influenza vaccinations, understand the potential role of an adherence measure in non-cycled oral antineoplastics, and estimate the potential impact of a value-based formulary.
Prajakta Waghmare, MS (Purdue University, USA) kicked off this session of podium presentations with a study evaluating the impact of medication synchronization (med-sync), which aligns patients’ chronic medication pick-up dates on a common date, on healthcare resource utilization (HCRU) and costs. The study team conducted a retrospective cohort study of Medicare beneficiaries previously enrolled in a med-sync program who were propensity score-matched to patients who did not participate in a med-sync program. Difference-in-difference analyses were conducted to determine whether the initiation of med-sync had an effect on HCRU overall (eg, outpatient, inpatient, emergency, and pharmacy). The authors found a significantly lower increase in outpatient visits, emergency department visits, and pharmacy use among the med-sync cohort compared to standard, but there was no significant difference in healthcare costs due to med-sync.
The presentations continued with Jacinda Tran, PharmD, MBA (Comparative Health Outcomes, Policy, and Economics (CHOICE) Institute, USA), who presented a study characterizing the trends in pharmacist-administered influenza vaccinations in the IBM MarketScan Commercial database between 2008 and 2020. The authors observed an overall increase in influenza vaccinations across all states throughout the study period, with notable increases in the proportion of influenza vaccinations administered at pharmacies. They concluded that public perception of pharmacists is changing and that pharmacist-administered vaccinations are becoming more widespread. Further, in a case study using a controlled interrupted time series analysis, the authors did not observe a significant effect of removing a policy in Montana requiring pharmacists to have a collaborative practice agreement in place in order to administer vaccinations.
The oral presentations continued with a study by Francis Staskon, PhD (Walgreens, USA), which utilized IBM MarketScan Commercial Claims and Encounters databases from 2017 to 2019 to establish proportion of days covered (PDC) as a measure of utilization for non-cycled antineoplastics and to examine the costs and outcomes associated with PDC of 80% or higher. The study found that PDC as an adherence measure was significantly associated with annual cost and utilization outcomes. Adherence (PDC >80%) was associated with higher drug costs, lower medical costs, fewer hospitalizations, and shorter oncology-related length of stays. The authors conclude that PDC may be an appropriate methodology to measure non-cycled cancer therapies.
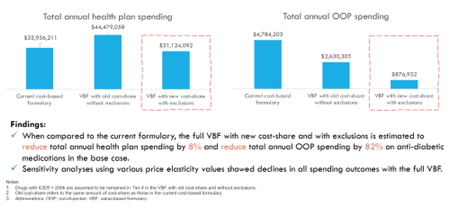
In the fourth presentation, Yilin Chen, MPH (Comparative Health Outcomes, Policy, and Economics (CHOICE) Institute, USA) presented a study on “Designing a Value-Based Formulary for Kaiser Permanente Washington: A Hypothetical Case Study of Diabetes Medication.” The authors designed a value-based formulary (VBF) for patients with diabetes mellitus at Kaiser Permanente Washington, and drugs with higher assessed value were assigned lower copayments and lower value were subjected to higher copayments. Chen and colleagues modeled the health plan’s potential annual drug costs and members’ out-of-pocket costs with the VBF compared to the current formulary, and the VBF was estimated to reduce payer costs by 8%, or $71 per member per year in annual costs, and $97 per member per year in out-of-pocket costs (Figure). They concluded that designing a VBF in a US employer-based health plan has the potential to save money for both the plan’s and the patient's out-of-pocket medication expenses.
Figure. Estimated health plan spending and patient out-of-pocket costs for antidiabetic medications versus value-based formularies (2019-2020)