Are We Patient and Care-Partner Centric Enough in Early Alzheimer’s Disease Clinical Trials?
Trupti Dhumal, MS, BPharm, West Virginia University, Morgantown, WV, USA
With regards to the current evolution in Alzheimer’s disease (AD), drug development—from later-stage symptomatic AD to disease-modifying monoclonal antibody (MAB) therapies—the treatment shift has experienced some mixed reviews. The new treatment pathways have been losing its essence of valuing patient relevance due to its increasing focus on biomarkers and cost. It is critical to evaluate whether the clinical outcome assessments (COA) account for patient relevant concepts in mild cognitive impairment and early AD trials for the new MAB therapeutics (Figure1).
Figure 1. Session agenda and speakers.

Taking into account the current issue, today’s session moderator John Harrison, PhD (Vrije Universiteit, Amsterdam) kicked off an interesting workshop focused on evaluating the COA measures in mild cognitive impairment and early AD trials and exploring the extent to which legacy measures account for patient relevant meaningful benefit. He introduced the other 3 presenters: William Herring, Sarah Acaster, and Russ Paulsen (UsAgainstAlzheimer’s).
Harrison gave a comprehensive background on the etiology of AD and mild cognitive impairment in early AD and shifted the discussion about how traditional assessments have low reliability and lack content validity.
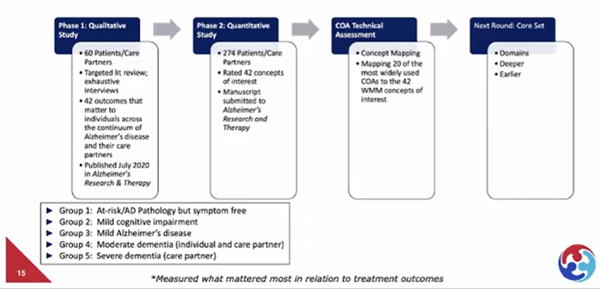
Russ Paulsen,MA (UsAgainstAlzheimer’s) took over the next part of the presentation and introduced the AD-PACE initiative. He shed light on aspects that matter most to the patient. The AD-PACE initiative qualitatively assessed elements important for AD patients and care-partners (Figure 2). Thirty-five items were rated being very or extremely important. A few of the concepts were related to taking medications correctly, not feeling anxious, using the bathroom, and not feeling like a burden. The next aim of the initiative was to create recommendations of COA for each patient group.
Figure 2. Study phases of AD-PACE research.
Sarah Acaster, MSc, BSc (Acaster Lloyd Consulting, Ltd, UK) continued the discussion on measuring and interpreting patient relevant outcomes. Developing a patient-relevant approach was the main emphasis of her talk. She discussed the discrepancies in the current COA’s by comparing them and suggested the inclusion of iADRS using anchor and distribution-based methods.
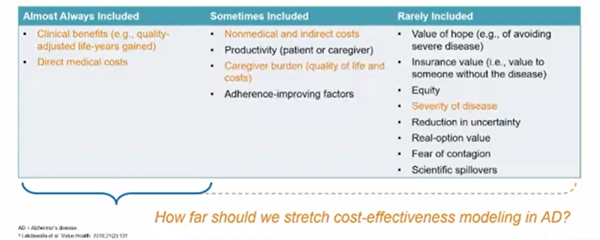
Lastly, William Herring, PhD (RTI Solutions, USA) highlighted ways to leverage the clinical trial outcomes to support long-term benefits in AD. He shed light on the concept of model-based value assessment and elements of value that are missing from current cost-effectiveness models (Figure 3). “If we take into account the value drivers, we can observe a disconnect on where we are measuring endpoints in clinical trials and where we think the clinical burden is. We have to find the right endpoint here and look to develop better endpoints,” said Herring. Moving forward his suggestion was to logically argue if the endpoint is a direct clinical benefit or a surrogate endpoint and to step outside the typical clinical trial models.
Figure 3. Limitations of traditional cost-effectiveness-based value assessment.
The interesting part of the entire discussion was that all the presenters included frequent polling questions to increase participant engagement.

