When Patients Take Charge of Their Quality of Life
Section Editors: Soraya Azmi, MBBS, MPH, Beigene, USA; Agnes Benedict, MSc, MA, Evidera, Budapest, Hungary
A Novel Patient-Derived Conceptual Model of the Impact of Celiac Disease in Adults: Implications for Patient-Reported Outcome and Health-Related Quality-of-Life Instrument Development
Leffler DA, Acaster S, Gallop K, Dennis M, Kelly CP, Adelman DC
Value Health. 2017;20(4):637-643.
https://www.valueinhealthjournal.com/
Celiac disease, a chronic inflammatory disease affecting the gut, can be severely debilitating in terms of its effect on patients unless managed by a gluten-free diet (GFD). It affects 1% of the population of the United States and Europe. Although the GFD can be effective, adhering to the strict dietary measures required can be a burden on patients. The combination of the symptoms of celiac disease and the GFD are highly impactful on patients’ health-related quality of life (HRQOL).
To assess HRQOL, there are disease-specific instruments currently in use: the Celiac Disease Questionnaire, the Celiac Symptom Index, and the Celiac Disease Quality of Life (CD-QOL). However, these were developed from items identified through literature reviews or clinical experts rather than from patient inputs. The study described by Leffler, et al describes a method of exploring the impact of celiac disease and GFDs on HRQOL as experienced by patients and describes how a conceptual model was derived through qualitative patient interviews.
The study followed the US Food and Drug Administration’s Patient-Reported Outcome Measures Guidance for Industry (2009) and informed the development of 3 celiac-specific outcome measures: the Celiac Disease Symptom Diary, the Impact of Celiac Disease Symptoms Questionnaire, and the Impact of Adhering to a Gluten-Free Diet Questionnaire. The study design was a cross-sectional qualitative study with the sample size being determined by data saturation (the point at which no new information is obtained by new data) rather than a prespecified sample size. Patients were recruited from a celiac disease center in Boston and patients’ medical charts were reviewed to ascertain whether inclusion criteria were met. Eligible patients who were 18 and older were then contacted to ascertain their interest in participating in the study. Semistructured interviews were then conducted one-on-one in person where possible and interviews were conducted by the same expert interviewer.
Figure 1. Celiac disease conceptual model. The blue boxes show the areas of impact caused by the concepts in gray boxes, the arrows indicate the direction of influence, and the dotted arrow represents a potential moderating factor.
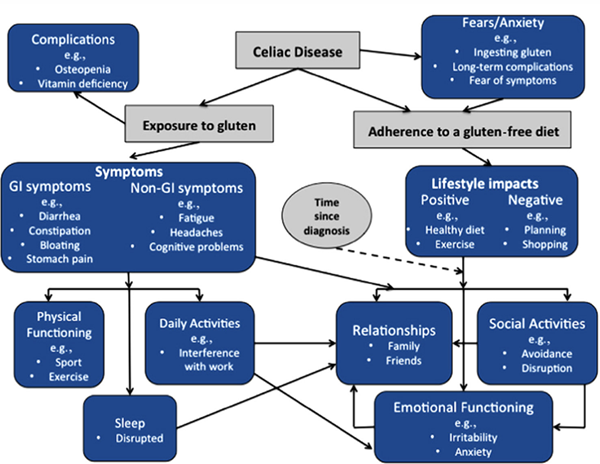
The data set was then coded and analyzed by experienced qualitative researchers and data were analyzed using thematic analysis. This involved an initial reading and rereading of the data to identify themes and categories, as well as to identify relationships between symptoms and impact. Qualitative analysis software was used to facilitate this process. Emergent themes and concepts were monitored with coding concordance assessed by a second coder who analyzed all the transcripts. The 2 coders met along with another team member to discuss and reconcile differences. This process continued until concept saturation was achieved. The codes and concepts identified were developed into a conceptual model upon review by all authors and an expert panel of 4 celiac disease clinical experts.
Twenty-one patients participated in the study, at which point the data saturation had been reached. The mean age was 42; 71% of the participants were women and 91% Caucasian. Qualitative analysis identified the themes that impact the HRQOL of patients with celiac disease as being as follows (Figure 1): fears and anxiety, day-to-day management of celiac disease, physical functioning, sleep, daily activities, social activities, emotional functioning, and relationships. Overall rate of adherence to a GFD was 90.5%.
Highlights of the findings and themes that were identified show that celiac disease can have a significant impact on how everyday life is experienced by patients. For example, abdominal pain, nausea, and bodily pain prevented patients from going shopping and interfered with work and study.
In terms of social activities, participants reported difficulties with eating out, worrying about whether restaurant kitchens could prepare a GFD meal appropriately. Sometimes that meant that participants would choose to avoid social outings.
Participants also felt depression and anxiety due to the symptoms, causing frustration with themselves. Similarly, in relationships there were times when having to discuss their need to adhere to a GFD caused some family or friends to show a lack of understanding or annoyance.
Aside from gathering evidence directly from patients to develop the new HRQOL instruments, this study was the first to attempt to measure the impact of adhering to a GFD. This clearly is an important part of managing the disease, which improves symptoms at the same time as it is particularly burdensome on patients’ lives. This shows that a key feature of patient centeredness may have been missing from prior HRQOL instruments.
The article highlights the role that patients can play in research that feeds into decision making about their well-being. It would be worth a visit to readers who are interested in ways in which patients themselves can be involved in the process of developing HRQOL measurements. The study was timely and highly appropriate given that in recent years, the role of the patient’s voice is being increasingly recognized as important in making well-informed and widely accepted decisions that can improve patient treatment and quality of life outcomes.

