The Value of Suicide Prevention: An Evidence-Based Call for Action
Long Khanh-Dao Le, PhD, Dai Quy Le, Monash University, Melbourne, Australia; Amanda Neil, PhD, University of Tasmania, Tasmania, Australia; Karl Andriessen, PhD, Jane Pirkis, PhD, University of Melbourne, Melbourne, Australia; Cathrine Mihalopoulos, PhD, Monash University, Melbourne, Australia; Lennart Reifels, PhD, University of Melbourne, Melbourne, Australia

Self-harm and suicide represent a global crisis.1 With suicide ranking among the leading causes of death across age groups and regions, the imperative for effective prevention strategies is clear.1 Suicide prevention is a vital public health priority that can foster hope in communities. Implementing interventions for suicide prevention is essential because it provides timely support to individuals who may be at risk, helping to reduce the likelihood of self-harm or a suicide attempt. Every life lost to suicide can leave behind a ripple of grief and unanswered questions, affecting families, friends, and society at large. Suicide prevention is not only about saving lives but also affirming that every life matters and that no one should face their struggles alone.
Yet effectiveness alone is not enough, interventions must also be economically viable to ensure scalability and sustainability.2
Without cost-effectiveness, even the most promising suicide prevention intervention could be limited to pilot programs or short-term initiatives, unable to reach the broader populations that need them most. Economic viability ensures that resources—whether in the form of public funding, healthcare budgets, or community investments—can be allocated wisely and consistently over time. Moreover, economically sustainable models allow for continuous improvement and adaptation to evolving needs, making suicide prevention interventions not just a reactive measure but a long-term commitment to public health equity. This article examines the economic case for suicide prevention and outlines actionable steps to enhance its value.
Suicide prevention is not only about saving lives but also affirming that every life matters and that no one should face their struggles alone.
Cost-Effective Pathways to Suicide Prevention: Global Evidence
The most recent systematic review of economic evidence for suicide prevention offers a timely and rigorous synthesis of the cost-effectiveness landscape in suicide prevention, which was presented in May 2025 at the ISPOR annual conference for health economics and outcomes research in Montreal, Canada.3 The review found more than 60 full economic evaluations or return-on-investment (ROI) studies across more than 20 intervention types.
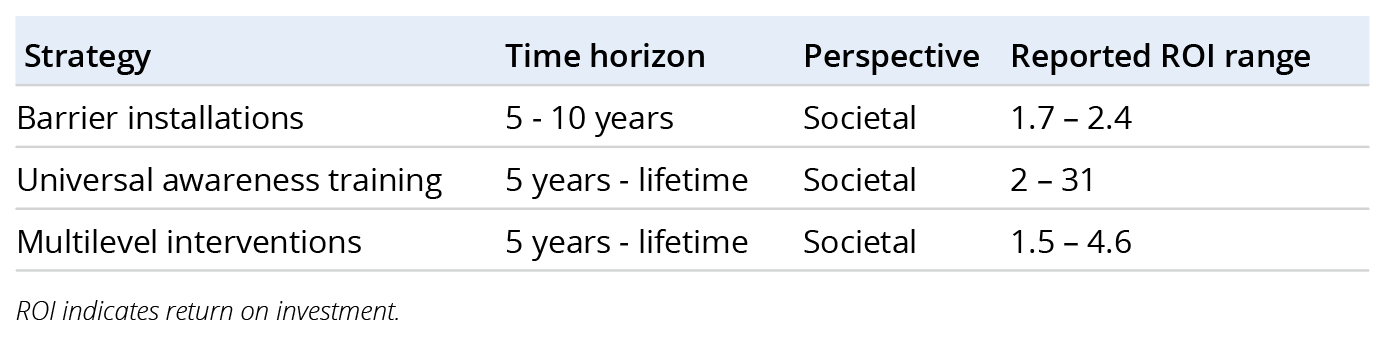
Universal interventions that apply to entire populations regardless of risk level include means restriction (eg, limiting access to suicide locations or pesticides) and awareness training. These interventions are often low cost and high impact (Tables 1 and 2). For example, barrier installations at known suicide locations mostly demonstrated favorable cost-effectiveness, with reported ROIs ranging from 1.7 to 2.4 or incremental cost-effectiveness ratios (ICERs) of $6500 - $103,000 per disability-adjusted life year (DALY) averted, whereas pesticide access restriction only cost between $110 and $4800 per life year saved.3 Similarly, awareness training—particularly for gatekeepers like teachers, police officers, and healthcare providers—also yielded positive ROIs, mostly ranging from 2 to 31 from a societal perspective.3
Table 1. Return on Investment for Select Suicide Prevention Strategies3
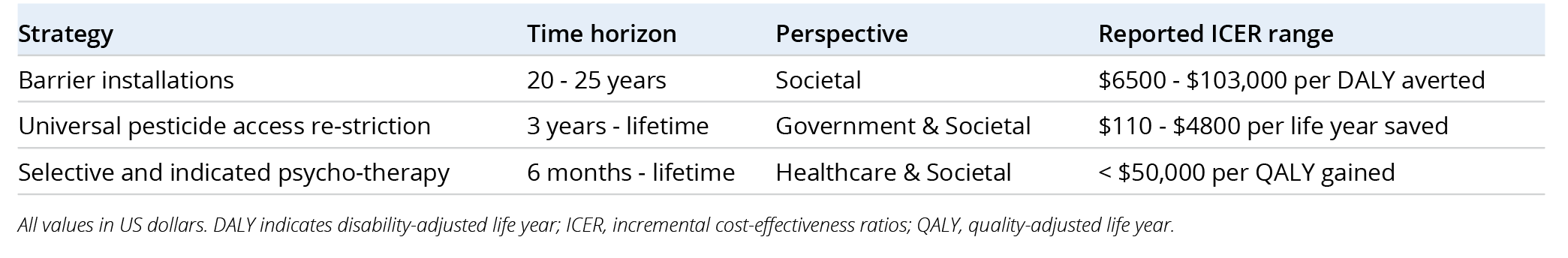
Targeted interventions encompass 2 key approaches: selective interventions, which aim to support individuals at heightened risk such as those diagnosed with mental health conditions, and indicated interventions, which are designed for individuals already showing signs of self-harming behavior. Psychotherapy, especially cognitive behavioral therapy (CBT), emerges as a standout across such strategies (Table 2). Twenty-two studies evaluated psychotherapy, with most finding it cost-effective (eg, ICERs < US$50,000 per quality-adjusted life year [QALY] gained) or cost-saving (eg, ICERs < $0 per QALY gained).3 Support services, such as crisis helplines and peer support programs, also show promise. These interventions have been shown to have substantial benefits in terms of reduced hospital admissions and/or length of stay, together with improved quality of life. Medication, although less frequently studied, appears cost-effective in specific contexts, particularly when combined with psychosocial support.3
Table 2. Cost-Effectiveness of Select Suicide Prevention Strategies3
Multilevel interventions combine elements from all 3 categories and are often implemented at the community or national level. These include comprehensive suicide prevention programs that integrate public awareness, clinical screening, and follow-up care. While complex and resource-intensive, multilevel interventions also demonstrated positive ROIs, ranging from 1.5 to 4.6 (Table 1), due to their broad reach and synergistic effects.3
Limitations in Economics of Suicide Prevention Research
Despite bearing a significant share of the global suicide burden,1 low- and middle-income countries remain underrepresented in economic evidence of suicide prevention.3
The current economic evidence has clear implications for suicide prevention. First, decision makers need to continue to prioritize proven cost-effective interventions including psychotherapy, support services, and means restrictions. These interventions should be scaled up, especially in high-income countries where infrastructure exists. Furthermore, multilevel strategies combine universal, selective, and indicated interventions into a cohesive framework, addressing suicide risk across the entire population while also targeting vulnerable groups.
Decision makers need to continue to prioritize proven cost-effective interventions including psychotherapy, support services, and means restrictions.
Evidence shows that such comprehensive approaches yield high ROI, not only by reducing suicide rates but also by potentially lowering healthcare costs associated with self-harm, which often require intensive inpatient and outpatient care (eg, emergency care, mental health care).3 In addition, these strategies may reduce productivity losses by preventing work absence (absenteeism), reduced on-the-job performance (presenteeism), and premature death among those with self-harm and suicidal behaviors.3 Investing in these holistic models demonstrates a strong commitment to long-term public health equity and resilience, even though they may require substantial upfront resources.
In this systematic review,3 most economic evaluations were conducted in high-income countries, limiting the generalizability of existing findings to low-middle income countries (LMICs), where 77% of deaths by suicide occur.6 To address this evidence gap, funding agencies, global health organizations, and academic institutions should prioritize research in LMICs to identify cost-effective, culturally relevant interventions. This includes supporting local data collection, capacity-building for researchers, and partnerships with community stakeholders. Expanding the evidence base in these regions is essential for designing scalable strategies that reflect real-world constraints and maximize impact.
Children and older adults face unique risk factors for suicide, yet they are often overlooked in economic evaluations and intervention design. In this review, only 18 studies focused on children and adolescents, and none specifically targeted older adults.3 For children and adolescents, school-based programs, peer support initiatives, and early screening can be promising for future research.5,6 Older adults, on the other hand, may benefit more from interventions that address social isolation, chronic illness, and financial security such as community engagement programs and integrated geriatric care.7
Dedicated research efforts are needed to understand the cost-effectiveness of age-appropriate strategies and ensure that suicide prevention is inclusive across the lifespan. Tailoring interventions to these groups has the potential to not only improve outcomes but also promote equity in public health.
References
- GBD 2021 Suicide Collaborators. Global, regional, and national burden of suicide, 1990–2021: A systematic analysis for the Global Burden of Disease Study 2021. Lancet Public Health. 2025;10(3):e189-e202. doi: 10.1016/S2468-2667(25)00006-4
- Krebs E, Nosyk B. Cost-effectiveness analysis in implementation science: A research agenda and call for wider application. Curr HIV/AIDS Rep. 2021;18(3):176-185. doi: 10.1007/s11904-021-00550-5
- Le L, Le DQ, et al. EE485 Economic evaluations of preventive interventions for self-harm and suicide: A systematic review. Value Health. 2025;28(6):S151. doi: 10.1016/j.jval.2025.04.2081
- WHO Global health estimates: Leading causes of death. Geneva: World Health Organization. https://www.who.int/data/gho/data/themes/mortality-and-globalhealth-estimates/ghe-leading-causes-of-death. Published August 2024. Accessed January 20, 2026.
- Marshall T, Cosgrove J, et al. Suicide prevention interventions in schools: assessing the evidence base. Psychiatr Serv. 2025;76(10):898-905. doi: 10.1176/appi.ps.20250162
- Schlichthorst M, Ozols I, Reifels L, Morgan A. Lived experience peer support programs for suicide prevention: A systematic scoping review. Int J Ment Health Sys. 2020;14(1):65. doi: 10.1186/s13033-020-00396-1
- de Mendonça Lima CA, De Leo D, Ivbijaro G, Svab I. Suicide prevention in older adults. Asia-Pac Psychiatry. 2021;13(3):e12473. doi: 10.1111/appy.12473

