Cost-Effectiveness of WIC Eligibility Extension for Preventing Maternal Postpartum Depression
Melody C. Ucho, MSPH, School of Public Health and Information Sciences, University of Louisville, Kentucky, USA

For more than 50 years, the Special Supplemental Nutrition Program for Women, Infants and Children (WIC) has responded to the health and nutrition needs of low-income families in the United States. The program currently serves more than 6 million adults and children.1 There has been compelling evidence of the impact of WIC in narrowing inequities imposed by socioeconomic status. For example, among children from low-income families, those whose parents are enrolled in WIC have higher assessment scores on cognitive function at age 2 years and are more likely to receive immunizations and consume nutritious foods compared with those whose parents are not enrolled.1 Despite robust evidence of WIC’s benefits for children, the underlying maternal mechanisms through which the program influences these outcomes remain insufficiently understood.
Maternal postpartum depression (PPD), one type of Perinatal Mood and Anxiety Disorders (PMADs), occurs within the first year after childbirth and affects 1 in 8 women in the United States.2 More than 45% of mothers with PPD experience suicidal ideation.3 In the United States, maternal mental health (including PPD) was reported to be one of two leading causes of postpartum deaths in 2020.4 Additionally, PPD impacts children and has been associated with low infant weight, increased episodes of childhood illnesses and generally low quality of life among infants.5
PPD has a sustained effect as an infant grows and develops. The impact of PPD can be observed in motor control, language, and emotional development delays among children in the first year of life. Furthermore, mothers affected by PPD experience loss in economic output due to work absenteeism and resultant unemployment. Mothers with PPD also report difficulty with initiation and continuation of breastfeeding, which may serve as a pathway for infant-mother bonding.6 Mechanistically, breastfeeding may confer psychological benefits through hormonal effects (oxytocin and prolactin), increased maternal self-efficacy, and strengthened mother–infant bonding. Empirical evidence suggests that these neuroendocrine mechanisms lower stress responses and decrease the likelihood of PPD.7 Furthermore, sustained breastfeeding has been associated with lower odds of PPD while early breastfeeding challenges are associated with higher depressive symptom scores.8,9
In 2017, untreated perinatal mood and anxiety disorders cost the United States an estimated $14 billion, driven by the cost of maternal care, lost productivity, and child health needs.
PPD is associated with longer hospital stays, more outpatient and emergency department visits, and weeks of drug therapy.10 In 2017, untreated PMADs cost the United States an estimated $14 billion, driven by the cost of maternal care, lost productivity, and child health needs.11 A 2023 report estimated $48 million in total societal costs, including $36 million from untreated PMADs and $6 million for child developmental disorders.12 Medicaid, covering more than 41% of US births, remains the largest payer for maternal mental health and spends an estimated $6747 per case involving treatment for PMADs and approximately $762 per individual over 5 years for PPD counseling.11,13 These data represent the grim reality of the human burden and the fiscal toll of untreated PPD and PMADs in general, but they also underscore that primary prevention can be an opportunity for fiscal payoffs.
Federally funded programs such as WIC and Medicaid offer an opportunity for primary care that includes social support, lactation counseling, and regular contact with health and social services that promote breastfeeding, reduce isolation, and expedite referral for mental health needs. WIC has historically differentiated postpartum eligibility by breastfeeding status: As represented in Figure 1, breastfeeding mothers have traditionally been eligible for up to 12 months of benefits, whereas non-breastfeeding mothers are eligible for shorter periods (commonly up to 6 months).14 The practical effect is that breastfeeding mothers get prolonged program engagement and access to counseling, which may influence depression risk through multiple pathways.15 However, it is important to note that this differentiation may selectively exclude women whose PPD and associated risk factors are barriers to breastfeeding.
Figure 1. PRAMS-based analysis: Identifying WIC eligibility based on breastfeeding status
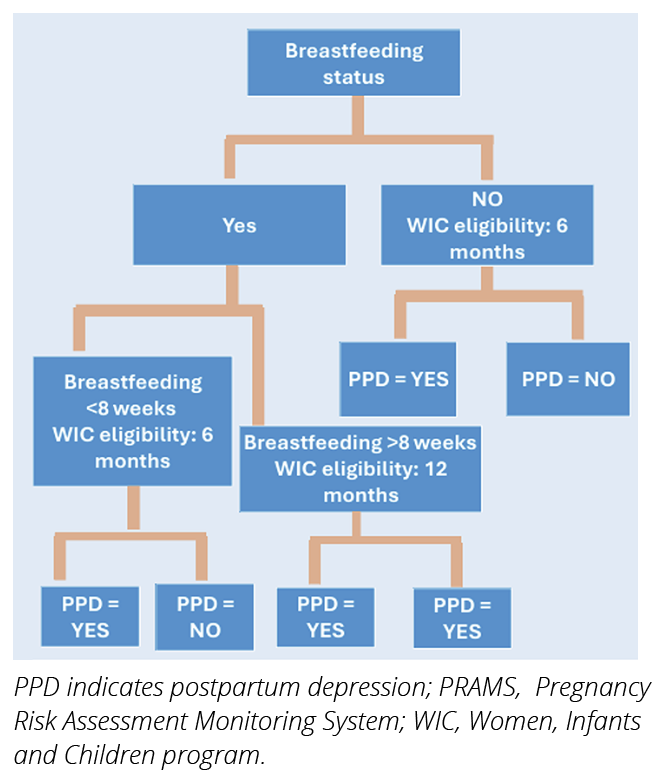
WIC already incentivizes breastfeeding as one key mechanism for PPD prevention; extending eligibility to 12 months for all new mothers, regardless of breastfeeding status, will also leverage a second key mechanism: an extended system of support. Extended participation in WIC offers repeated contacts with available support and resources during the postpartum period, including nutrition education, lactation support, perinatal depression screening, and connections to community resources—all factors that can promote maternal well-being and reduce the likelihood of PPD. But, in addition to clinical evidence of improved outcomes, informed fiscal decisions about expanding maternal WIC eligibility for all new mothers will depend on empirical evidence of the estimated amount of money that would be saved by payers, such as Medicaid, as a result of the change.
My study16 presents new evidence indicating that extending WIC eligibility from 6 to 12 months for new mothers, regardless of breastfeeding status, may be a highly cost-effective strategy to prevent and address PPD. Using data from the Pregnancy Risk Assessment Monitoring System (PRAMS) (2016–2022) and the US Department of Agriculture (USDA)-reported WIC unit costs (cost per woman), as shown in Figure 2, I found that mothers effectively eligible for 12 months of WIC (proxied by breastfeeding for more than 8 weeks) had lower likelihood of reporting PPD. This translates to a cost of approximately $447 per woman for each percentage-point reduction in PPD risk.
Figure 2. PRAMS-based comparison of PPD cases by duration of participation and WIC costs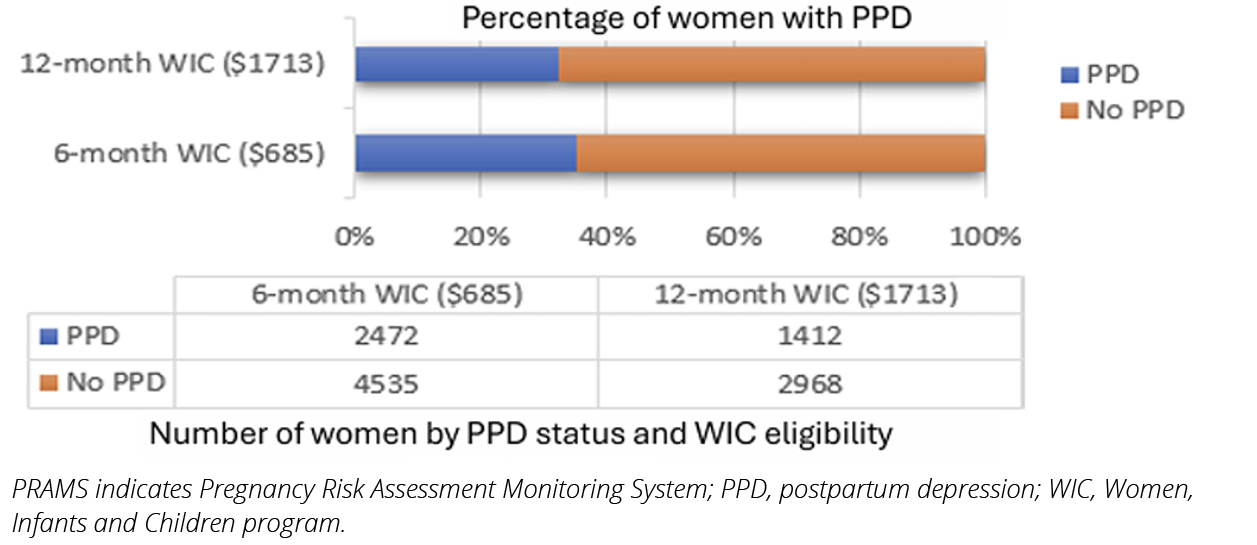
To interpret the study findings in context, WIC eligibility extension to 12 months will cost approximately $4 per PPD case averted. Given the previously mentioned treatment costs per woman for PPD incurred by Medicaid and population-level estimates of treatment burden, the per case cost of prevention implied by this study is low relative to the expected benefit and would also suggest similarly low relative costs of prevention per woman, a high return on prevention investment, and the reduction or elimination of associated clinical and societal costs of PPD. Wilkinson et al estimated that a hypothetical intervention in which physicians were compensated for screening new mothers for PPD would cost $943 per woman and $10,182 per PPD case in remission.17 My findings suggest extending WIC eligibility is potentially a much more cost-effective approach.
This evidence underscores several pragmatic actions for WIC program leaders and policy makers, and can potentially inform legislative propositions such as the Wise Investment in Our Children Act and the Black Maternal Health MOMNIBUS Act, which have hitherto received limited traction.18,19
Strengthening WIC’s capacity to screen for depressive symptoms by using validated tools to provide psychosocial interventions and streamline referrals to behavioral healthcare could transform routine nutrition visits into powerful preventive encounters.
First, cost-effectiveness analysis suggests longer eligibility could prevent cases of PPD, which would reduce downstream treatment expenditures. In addition, given the higher PPD prevalence of 19.8% among women who are eligible and participating in WIC compared to non-participating (16.3%) or non-eligible (6.8%) counterparts,20 integrating mental health services within WIC should be prioritized. Strengthening WIC’s capacity to screen for depressive symptoms by using validated tools to provide psychosocial interventions and to streamline referrals to behavioral healthcare could transform routine nutrition visits into powerful preventive encounters. This approach would include eliminating fragmentations in the implementation of helpful programs and instituting a mandate for nationwide adoption.
Although my findings provide a strong foundation for stakeholder engagement by showing lower prevention costs per woman and the potential to avert clinical and societal costs of PPD, causal inference should be made cautiously. PRAMS data are observational, and breastfeeding duration served as a proxy for WIC participation, assuming continuous enrollment. Reverse causation and unmeasured confounding are possible, and cost estimates, based on 2016 USDA WIC data, may not reflect local variations. Nonetheless, the results align with independent evidence demonstrating the positive effects of WIC’s resources on maternal health, measured using the web-based Breastfeeding Savings Calculator developed by the US Breastfeeding Committee.15 These benefits could be expected to increase with extended participation in the WIC program.
Enhanced data linkage across WIC, Medicaid, and maternal health databases like PRAMS is essential for monitoring outcomes and ensuring evidence-based improvement. Maternal health innovation programs such as Perinatal Quality Collaboratives,21 the Maternal Opioid Misuse Model,22 and PRAMS–Medicaid linkages23 show the value of cross-system integration. Extending WIC to 12 months with mental health screening, lactation support, and linked data evaluation represents a scalable, equity-sensitive policy with both immediate and long-term returns, one that advances public health and fiscal responsibility.
References
- Carlson S, Llobrera J, Neuberger Z. WIC Works: A Cost-effective Investment in Improving Low-income Families’ Nutrition and Health. Center on Budget and Policy Priorities; 2025. https://www.cbpp.org/research/food-assistance/wic-works-a-cost-effective-investment-in-improving-low-income-families Published October 14, 2025. Accessed January 2, 2026.
- Bauman BL, Ko JY, Cox S, et al. Vital signs: postpartum depressive symptoms and provider discussions about perinatal depression — United States, 2018. Centers for Disease Prevention and Control (CDC). MMWR Morb Mortal Wkly Rep. 2020;69:575-581. doi: 10.15585/mmwr.mm6919a2.
- Chen C, Okubo R, Okawa S, et al. The prevalence and risk factors of suicidal ideation in women with and without postpartum depression. J Affect Disord. 2023;340:427-434. doi: 10.1016/j.jad.2023.08.051.
- Medicaid and CHIP Payment and Access Commission. Access in Brief: Postpartum Mental Health in Medicaid. MACPAC.org. https://www.macpac.gov/wp-content/uploads/2025/01/Access-in-Brief-Postpartum-Mental-Health-in-Medicaid.pdf Published January 2025. Accessed January 2, 2026.
- Dunkel Schetter C, Tanner L. Anxiety, Depression and stress in pregnancy. Curr Opin Psychiatry. 2012;25(2):141-148. doi: 10.1097/YCO.0b013e3283503680.
- Slomian J, Honvo G, Emonts P, Reginster J-Y, Bruyère O. Consequences of maternal postpartum depression: a systematic review of maternal and infant outcomes. Women’s Health (Lond). 2019;15:17. doi: 1745506519844044.
- Pope CJ, Mazmanian D. Breastfeeding and postpartum depression: an overview and methodological recommendations for future research. Depress Res Treat. 2016 Apr 11;2016:4765310.
- Alimi R, Azmoude E, Moradi M, Zamani M. The association of breastfeeding with a reduced risk of postpartum depression: a systematic review and meta-analysis. Breastfeed Med. 2022;17(4):290-296. doi: 10.1089/bfm.2021.0183.
- Watkins S, Meltzer-Brody S, Zolnoun D, Stuebe A. Early breastfeeding experiences and postpartum depression. Obstet Gynecol. 2011;118(2 Pt 1):214–221. doi: 10.1097/AOG.0b013e3182260a2d.
- Pollack LM, Chen J, Cox S, et al. Healthcare utilization and costs associated with perinatal depression among medicaid enrollees. Am J Prev Med. 2022;62(6):e333–e341. doi: 10.1016/j.amepre.2021.12.008.
- Luca DL, Margiotta C, Staatz C, et al. Financial toll of untreated perinatal mood and anxiety disorders among 2017 births in the United States. Am J Pub Health. 2020;110(6):888–896. doi: 10.2105/AJPH.2020.305619
- Platt IS, Pendl-Robinson EL, Dehus E., et al. Societal costs of untreated perinatal mood and anxiety disorders in Vermont. Arch Women’s Ment Health. 2024;27(4):585-594. doi:10.1007/s00737-024-01429-1
- Counts NZ, Kuklinski MR, Wong V, Feinberg ME, Creedon TB. Comparison of estimated incentives for preventing postpartum depression in value-based payment models using the net present value of care vs total cost of care. JAMA Netw Open. 2022;5(4):e229401. doi:10.1001/jamanetworkopen.2022.9401.
- United States Food and Drug Administration. “Special Supplemental Nutrition Program for Women, Infants and Children.” 50 Fed Reg 6121 (Feb 13, 1985). Codified at 7 CFR Part 246.7, Subpart C. https://www.ecfr.gov/current/title-7/subtitle-B/chapter-II/subchapter-A/part-246 Accessed January 2, 2026.
- Oliveira V, Prell M, Cheng X. Economic implications of increased breastfeeding rates in WIC. Amber Waves. United States Department of Agriculture. https://www.ers.usda.gov/amber-waves/2019/february/economic-implications-of-increased-breastfeeding-rates-in-wic Published February 14, 2019. Accessed January 2, 2026.
- Ucho M, Karimi S. Cost-Effectiveness of WIC Eligibility Extension in Preventing Maternal Postpartum Depression: US Payers’ Perspective [ISPOR Europe abstract EE173]. Value Health. 2025;28(12):S134.
- Wilkinson A, Anderson S, Wheeler SB. Screening for and treating postpartum depression and psychosis: a cost-effectiveness analysis. Matern Child Health J. 2017;21(4):903–914. doi:10.1007/s10995-016-2192-9
- National WIC Association. WIC Act Will Extend Eligibility Age and Improve Nutrition for Children and Mothers [press release]. Washington, DC: National WIC Association; May 16, 2023. https://www.nwica.org/press-releases/wic-act-will-extend-eligibility-age-and-improve-nutrition-for-children-and-mothers Accessed January 2, 2026.
- Black Maternal Health Caucus. The Momnibus Act: The Solution to America’s Maternal Health Crisis. https://blackmaternalhealthcaucus-underwood.house.gov/Momnibus Accessed January 2, 2026.
- Pooler J, Perry DF, Ghandour RM. Prevalence and risk factors for postpartum depressive symptoms among women enrolled in WIC. Matern Child Health J. 2013;17(10):1969-1980. doi:10.1007/s10995-013-1224-y
- United States Centers for Disease Control and Prevention. Perinatal Quality Collaboratives; May 15, 2024. https://www.cdc.gov/maternal-infant-health/pqc/index.html Accessed January 2, 2026.
- United States Centers for Medicare and Medicaid Services. Maternal Opioid Misuse (MOM) Model. https://www.cms.gov/priorities/innovation/innovation-models/maternal-opioid-misuse-model Accessed January 2, 2026.
- United States Department of Health and Human Services. Developing a Multi-State Network of Linked Pregnancy Risk Assessment Monitoring System (PRAMS) and Clinical Ourcomes Data for Patient-Centered Research. https://aspe.hhs.gov/developing-multi-state-network-linked-pregnancy-risk-assessment-monitoring-system-prams-clinical Accessed January 2, 2026.

